Our next clinical installment will touch a bit on trauma and burn care in Angola. It’s important to recognize that trauma (accidents, homicide, suicide, war) is the third largest killer of people on the planet (after cardiovascular and infectious diseases). But when you consider that trauma tends to prey on the young and the working members of societies, its impact is felt by all. Again, I’d like to give a glimpse by sharing a few clinical vignettes.
Head injury
Maria is 4 years old. 4 days before we met her, she was in a motor vehicle accident where she was thrown from the motorcycle she had been riding together with her parents (a very common practice as transport is expensive). Her scalp laceration was sewn up at a local health post. She was brought to the hospital 3 days later with fever, pus draining from her wound, and altered mental status. Her wound was drained by the ER nurses. Physical exam then revealed a depressed skull fracture. Steve took her to the operating room, where he elevated the compressed area.


Motor Vehicle Collisions
Back in November, as we were coming back from the coastal city of Namibe, we came upon this single-vehicle wreck on the side of the road. The driver we found face down in a ditch, laying in his own blood and vomit. To my surprise, and before we could take spine precautions, he scrabbled to his feet, reeking of alcohol and clearly head injured. A taxi van pulled up at that moment, and agreed to take him the rest of the way into the Namibe general hospital.


It’s not just bad decision making that makes for road vehicle accidents in the Global South. This vehicle was one of a dozen overturned trucks that Beth witnessed on her eye trip in December.

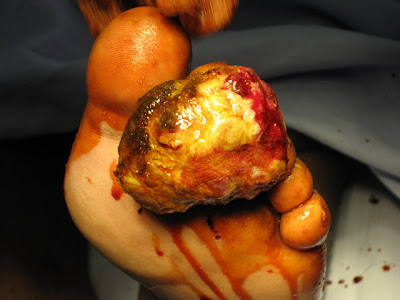
Burns
Burns are also a problem all too common in Angola today.
Felicia is three years old and was sleeping face down under a sheet which caught fire when a nearby candle fell on it. She sustained severe burns to her back, buttocks, arms, scalp, and some on her face. Her brother sleeping next to her died that night. She will need to undergo continued daily, and painful, dressing changes while her skin slowly grows back, as the conditions at this hospital in Kalukembe are unlikely to allow successful skin grafting at this stage.
Katarina, nineteen, was burned a year ago, when the thatched roof of her mud brick home caught fire and fell on her. Her skin was also allowed to merely grow back slowly with time. However, given the location of her burns, she developed contractures – debilitating scars from burns which impede normal movement – of her elbow, shoulder and chest wall. With skin grafting and simple reconstructive techniques, we were able to release her shoulder and elbow contractures. However, she will never be able to breastfeed.

Because of spartan living conditions and lack of electricity, burns disproportionately affect the poorer strata of our population here, as in most of the developing world, as demonstrated by both of these cases. The pain and disability keeps these individuals from being able to work and thus from being able to improve their lot. Seeing this has compelled me to work to improve the treatment of burned patients in this part of the world.
War
Angola suffered 27 years of civil after its independence in 1975. Thankfully, a lasting peace was established 5 years ago. But the scars of this conflict will take untold numbers of years to heal – for both the landscape and for human souls. Countless landmines (estimates between 500 thousand and 10 million) were placed during the war as a means of controlling population movements.
 These remain a deadly legacy to Angolans and a blight to development as otherwise arable fields linger untouchable. Fortunately, Angola’s government, together with Halo Trust, has been actively demining the countryside, and was recently applauded by member states of the Ottawa Anti-Personnel Landmines Convention for its efforts.
These remain a deadly legacy to Angolans and a blight to development as otherwise arable fields linger untouchable. Fortunately, Angola’s government, together with Halo Trust, has been actively demining the countryside, and was recently applauded by member states of the Ottawa Anti-Personnel Landmines Convention for its efforts.As with so many conflicts around the world, summary executions occurred right here in our backyard during the war years. These are the skeletal remains and uniform of someone thrown off the edge of nearby cliffs years ago. A sobering reminder, in such a beautiful place, of the atrocities of war.

Personal Violence
Gratefully, we have seen comparatively little intentional violence here in Lubango today. At the end of the war, demilitarization efforts succeeded in drastically reducing the number of small arms in country. Violence against women, however, remains largely undocumented and unrecognized. And violence in schools, though uncommon, does occur in Angola as well. Joaquim, 7 years old, was brought by his mother to the hospital with a 2 day history of an acutely swollen, draining eye, which started during school. He denied being attacked, but on operative exploration, it was clear a stick or a pencil had been shoved through the globe. His eye was destroyed, and it required an enucleation (removal of the eye). Next to him is Rob Mutter, a visiting Vanderbilt medical student, who we had the pleasure of hosting this last month.

This will be the last somber update. But we feel somber truths need to be spoken.
In personal news, we have only two weeks remaining of our time here in Lubango. Hence, we are simultaneously making preparations for our return to the US and our move to Boston, and investing in the relationships and work we’ve been given here. Thank you for journeying with us. Until the next update!
Beth and Robert